
No one wants to run into a health problem that they could prevent. Correctly timed screening tests can detect diseases or health disorders before symptoms show, helping you get ahead of problems earlier. They also give you a deeper ownership of your own state of well-being.
Early detection helps inform lifestyle changes and monitoring. These changes reduce the risk of disease and can significantly increase your chances of finding effective treatments. For example, cases of colorectal cancer in the United States have been declining by approximately 1% every year due to better awareness of screening and lifestyle choices—though this is largely a reflection of adults over 65. Rates for adults aged 50-64 have been rising, and the generally advised age for colonoscopy has dropped from 50 to 45 in recent years in hopes that early detection will also improve outcomes.
Generally, doctors advise people under 50 with no medical problems to have a check-in visit every three years to make a general assessment of health. Yet, about half of Americans have skipped or delayed medical care because the cost is a significant barrier. Other reasons are lack of awareness, insurance coverage issues, and lack of trust in service providers.
About eight out of every 10 adults in the United States visited a doctor as of 2020. The frequency of their visits depends on age and underlying health status. While this figure is encouraging, there remains a significant gap in screening frequency for older adults for several health conditions of concern. In an effort to plug that information gap, Guava Health outlines how frequently you should be screened for 10 health conditions and diseases, citing research from the Preventive Services Task Force, the Centers for Disease Control and Prevention, and medical journals.
Diabetes

Diabetes is a deceptively common disease; about one out of five people with diabetes are unaware that they have it. This makes screening for diabetes very important. Among U.S. adults, it is the leading cause of kidney failure and new cases of blindness, and is closely associated with increased risks of cardiovascular disease, nonalcoholic fatty liver disease, and nonalcoholic inflammation of the liver. The U.S. Preventive Services Task Force recommends screening every three years. This is especially advised for adults over 35 or people with one or more risk factors—particularly those who have obesity or are generally overweight. To make a diagnosis, a doctor takes a blood sample for an A1c test, which shows the average blood sugar level for two to three months.
High cholesterol
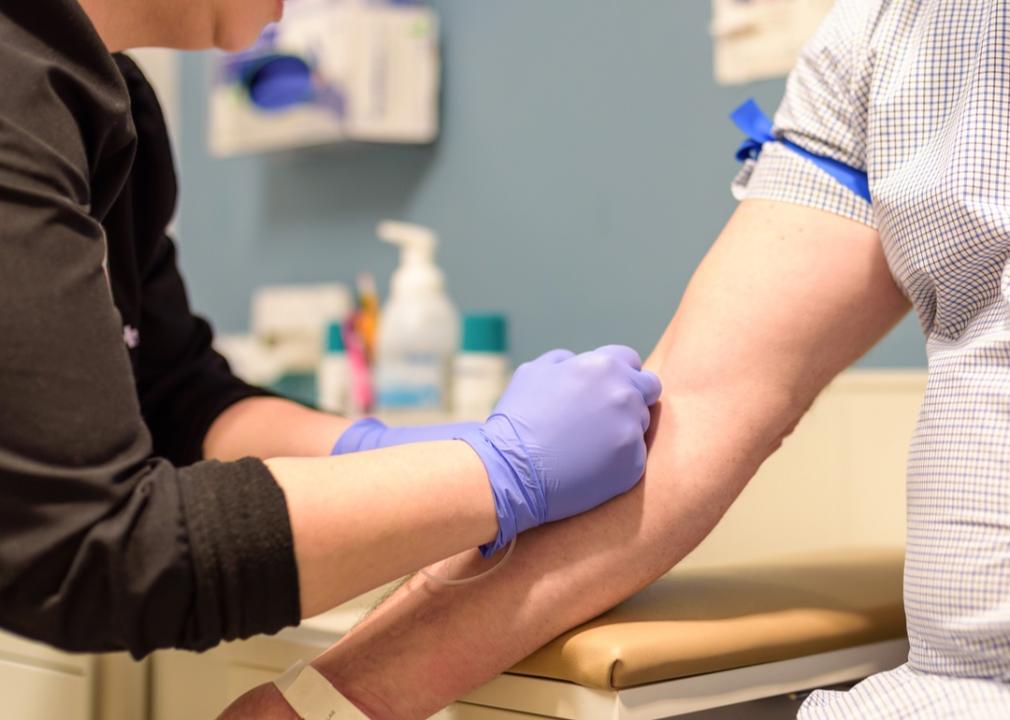
High blood cholesterol increases one’s risk of heart disease, the leading cause of death in the United States, as well as stroke. Unfortunately, high cholesterol is asymptomatic, which makes regular blood screening crucial to its detection and treatment. Children and teenagers should get their cholesterol levels checked at least once when they’re between ages 9 and 11 and then every five years thereafter. Doctors recommend that adults check their cholesterol levels every four to six years. People with conditions like diabetes or heart disease and those with a family history of high cholesterol are advised to get screened more frequently.
Chronic kidney disease

According to the Centers for Disease Control and Prevention, around one in seven American adults have chronic kidney disease. More alarming, the CDC estimates as much as nine of 10 adults do not realize they have the disease. Blood pressure monitoring, urinalysis, and blood tests help a doctor estimate a patient's glomerular filtration rate, or how well your kidneys are filtering waste. The United States Preventive Services Task Force reported that extra research is needed to recommend routine screening. Other sources like the National Kidney Foundation suggest annual tests.
Colon cancer

In the United States, colon cancer is the third most commonly diagnosed cancer in both men and women each year. To detect and prevent colon cancer early, routine screening should start at the age of 45. However, people with inflammatory bowel disease, a history of colon cancer, or a genetic disposition toward colorectal disease should start screening earlier. The United States Preventive Services Task Force suggests screening methods like stool tests, a CT colonography, a flexible sigmoidoscopy, or a colonoscopy.
Lung cancer
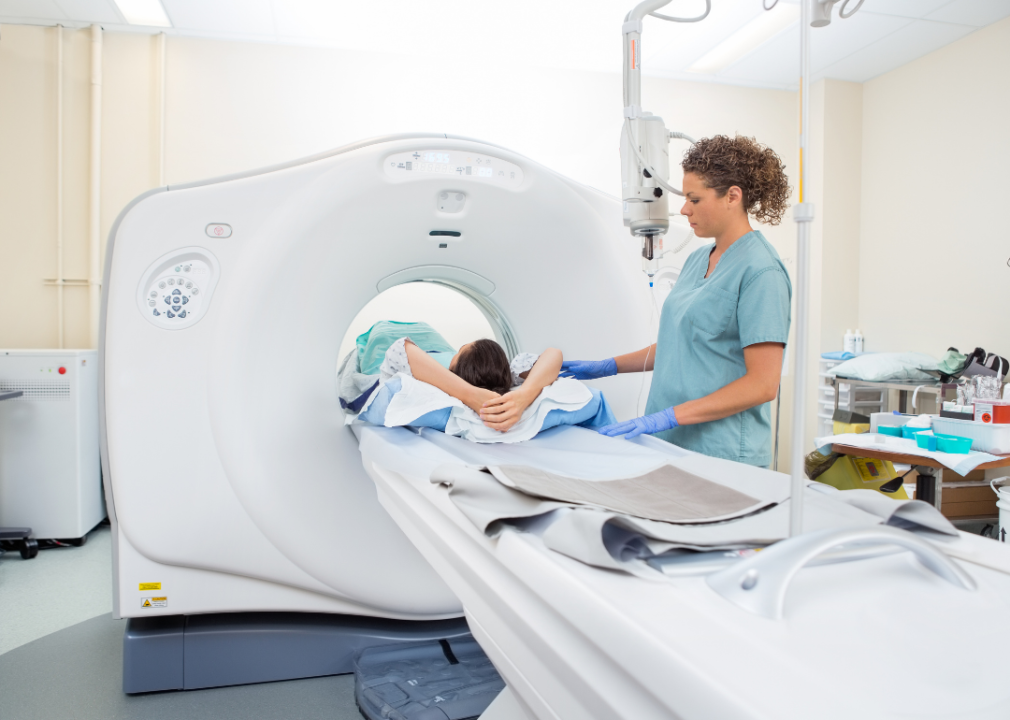
Lung cancer accounts for one in every four cancer deaths, making it the most common cause of mortality among cancer patients. According to the American Cancer Society, those with a smoking history—including those currently smoking or those who have quit in the last 15 years—should screen yearly with a low-dose CT scan through age 74. Those with a 30 pack-year smoke history are also advised to screen—a pack-year is defined as one year of smoking one pack of cigarettes each day. The United States Preventive Services Task Force gives a similar recommendation. They recommend screening for adults between the ages of 50 to 80 who have a 20 pack-year history.
Breast cancer

In the United States, breast cancer is the most common cancer diagnosed in women after skin cancer, which is generally quantified across multiple skin cancer forms. Breast cancer is commonly diagnosed in women between the ages of 55 and 64. According to the U.S. Preventive Services Task Force (USPSTF), age is the most important risk factor. Based on this, the USPSTF recommends women aged 50 to 74 with an average risk for breast cancer have a mammography once every two years. Other organizations suggest screening once every year or once every two years for women aged 50 and above. As women get older, the number of breast cancer deaths prevented by screening rises. Mammography and Magnetic Resonance Imaging (MRI) are the most common screening tests for breast cancer.
Cervical cancer

Human papillomavirus (HPV) is responsible for nearly half of all cervical cancers, and 80% of sexually active women will have this virus. This is the basis of the recommendations given for screening women for cervical cancer. The most common test performed to screen for cervical cancer in women is the Pap test, or Pap smear. As reported by the National Cancer Institute, the American Cancer Society (ACS) updated recommendations for cervical cancer screening in 2020. ACS recommends cervical cancer screening with an HPV test every 5 years for anyone with a cervix from age 25 to age 65. If HPV testing alone is not available, an HPV/Pap co-test every 5 years or a Pap smear every 3 years is recommended. One significant change to the ACS’ recommendation here is that the prior recommendation for a Pap test every three years for women ages 21-24 was removed.
High blood pressure

High blood pressure, also called hypertension, tends to have no symptoms and a diagnosis must be made by a medical professional. Testing for high blood pressure is important because the condition increases the risk of stroke. The American Heart Association considers blood pressure numbers within normal range if it measures 120/80 mm Hg—120 is how much pressure your blood pushes against your artery walls as it beats and the 80 indicates the pressure when it rests between beats. The association recommends screening tests for adults 20 years and older with blood pressure at or below the normal range every two years, with the frequency of follow-up depending on one’s risk level. More frequent screening tests are recommended when blood pressure is higher than normal range. An at-home kit is an efficient tool for monitoring your blood pressure—especially if you have high blood pressure.
Sexually transmitted diseases
This category comprises a number of diagnosable diseases, including but not limited to gonorrhea, chlamydia, hepatitis B and C, HIV, and syphilis. CDC recommendations vary for each. In general all people 13-64 should be tested for HIV at least once. Sexually active women younger than 25 years should be tested for gonorrhea and chlamydia every year, and pregnant women should be tested for syphilis, HIV, hepatitis B, and hepatitis C starting early in pregnancy, with additional tests as needed depending on risk factor. CDC further recommends all sexually active gay and bisexual men be tested yearly for syphilis, chlamydia, and gonorrhea, as well as HIV.
Overall in this category, screening recommendations are based less on age bracket than behavior, therefore regardless of age, adults over 45 should follow CDC guidelines based on their individual lifestyles.
Osteoporosis
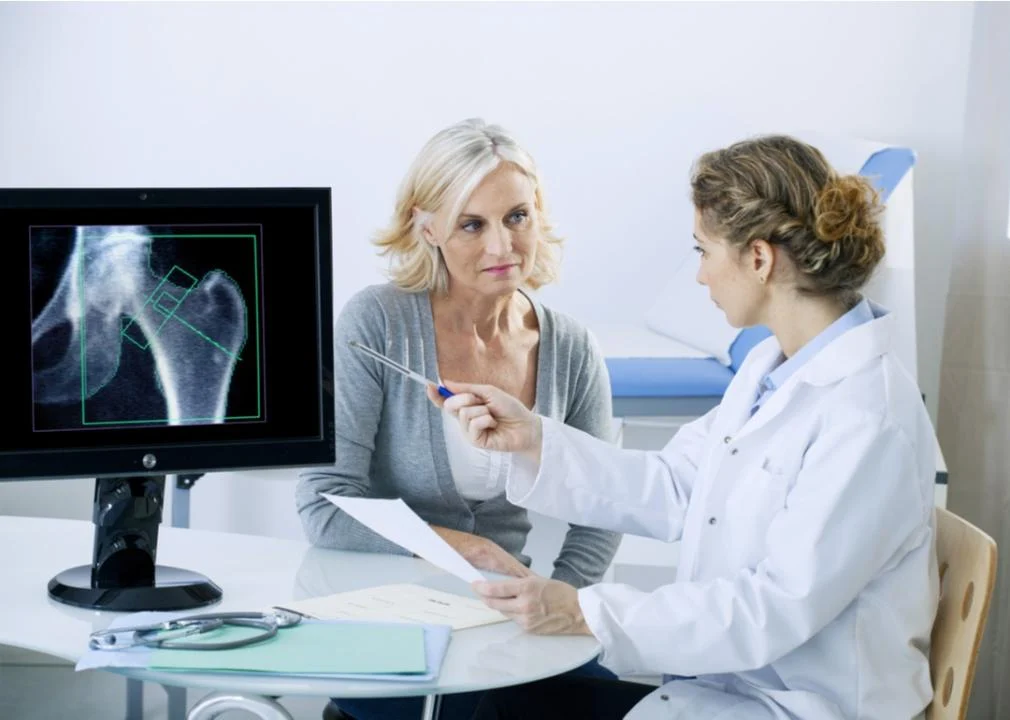
Osteoporosis is the most common bone disease in the United States and is most prevalent among women. It is brought on by low bone mass that leads to weakening of bone tissue, structure, and strength over time. A study reported by the National Institutes of Health showed that women 65 years and older with healthy bone density can have a screening interval of 15 years after their initial test. According to the United States Preventive Services Task Force, while there is limited evidence of the advantages of screening for osteoporosis in males, bone measurement testing to prevent osteoporotic fractures in women is strongly recommended. Other factors that can influence screening frequency include age-specific diseases or when patients take certain medications.





